Being familiar with common drugs and their antidotes is important for nurses. There are hundreds of known antidotes in the medical field nowadays but there are some in particular that need to be remembered because of how frequently they are used in times of emergencies. Being knowledgeable about antidotes is critical especially during times of emergencies so you can quickly reverse overdosage effects of the used drug.
What Is An Antidote?
The word antidote came from the Greek word “antididonai” which means “given against”. Antidotes have long been used since the ancient times.
Hundreds of years ago, potions and concoctions were formulated in apothecaries to treat poisons and stings. Nowadays, there is a wide range of antidotes made to counteract accidental or intentional overdosage in clinical settings.
Basic knowledge about antidotes is essential for nurses especially those who are working in acute care settings. To help you get started, here are some of the most common drugs and their antidotes:
Also Read: A Nurse’s Ultimate Guide to Accurate Drug Dosage Calculations
Acetylcysteine
Indication: Paracetamol, Carbon tetrachloride
Mode of Action: Protects against liver damage by enhancing production of glutathione thereby increasing microcirculation and increasing blood flow.
Dosage: Initial dosage is 150mg/kg in 200 mL of 5% dextrose through slow IV injection in a period of 15 minutes. Initial dose should be followed by 50mg/kg in 500 mL of 5% dextrose for 4 hours then 100mg/kg in 1000 mL of 5% dextrose for 16 hours.
Activated Charcoal
Indication: Most poisons
Mode of Action: Inhibits systemic absorption of toxin through its high adsorptive capacity.
Dosage: 50 gram orally every 4 hours until it appears in the stool for adult and 10-15 gram orally every 4 hours for children until it appears in the stool.
Amyl Nitrite
Indication: Cyanide
Mode of Action: Facilitates conversion of hemoglobin to methemoglobin to inhibit cyanide’s affinity to cytochrome oxidase enzymes thereby inhibiting its toxic effects.
Dosage: Ampoule contents should be inhaled for 30 seconds every minute. Use new ampoule every three minutes.
Atropine
Indication: Organophosphates and carbamate poisoning
Mode of Action: Inhibits the action of acetylcholine at the muscarinic sites to interrupt initial effects of organophosphate and carbamate poisoning.
Dosage: 2 mg through IV
Benzylpenicillin
Indication: Amatoxin poisoning
Mode of Action: Protects the liver by inhibiting entry of amatoxins into the hepatic cells.
Dosage: 600mg/kg on the first day and 300mg/kg on the second and third day
Calcium Gluconate
Indication: Hydrofluoric acid, calcium channel blockers and oxalates
Mode of Action: Increases calcium concentration to overcome calcium channel blockade in the cells and upkeep with depletion of calcium concentration in the system.
Dosage: 3grams for a 10% calcium gluconate that can be repeated every 10 to 20 minutes for a total of three to four doses
Cholestyramine
Indication: Anti-coagulants
Mode of Action: Inhibits the absorption of anti-coagulants in the system by forming non-adsorbable complex with bile acids in the intestines.
Dosage: 4 grams orally for up to three times daily
Cyanokit (Hydroxocobalamin)
Indication: Cyanide poisoning
Mode of Action: Binds with cyanide ions to facilitate excretion into the urine.
Dosage: 5 grams through intravenous infusion for 15 minutes
Dicobalt edetate
Indication: Cyanide toxicity
Mode of Action: Forms stable ion-complexes with cyanide to facilitate its excretion in the urine.
Dosage: 300mg through intravenous push for 1 minute followed by 50mL of 50% dextrose. Initial dose may be repeated if inadequate and can be further followed by a 300mg dose.
Dimercaprol
Indication: Arsenic, gold and inorganic mercury poisoning
Mode of Action: Binds with heavy metals to form dimercaprol-metal complex which can be readily excreted in the urine.
Dosage: 2.5mg – 3mg per kilogram weight through deep IM every four hours for two days then 2-4 times daily on the third day and 1-2 times daily for 10 days until recovery.
Ethanol
Indication: Ethylene glycol and methanol poisoning
Mode of Action: Inhibits formation of toxic metabolites so the toxic alcohol ingested can be excreted in the urine. It doesn’t directly affect the presence of the toxic metabolites that have already formed so hemodialysis is also recommended.
Dosage: Adult dosage for 5% ethanol is 2.76/mL/kg/hr either through oral or intravenous route
Flumazenil
Indication: Benzodiazepine overdose
Mode of Action: Acts on benzodiazepine receptors to block central effects of benzodiazepine.
Dosage: 0.2mg through IV for 30 seconds. If there is no response, 0.3mg can be given for another 30 seconds. Additional doses at 0.5mg at 30-60 second intervals until a total dose of 3mg is achieved.
Glucagon
Indication: Beta blockers, calcium channel blockers and hypoglycemic toxicity
Mode of Action: Increases myocardial contractility and heart rate similar to beta-agonist effects. It also decreases vascular resistance to improve cardiac output. Glucagon works on improving glucose levels by activating hepatic glycogen.
Dosage: 2-10mg through IV push and may be repeated as required for beta blocker and calcium channel blocker toxicity. For hypoglycemic toxicity, 1-2mg through intramuscular injection.
Methionine
Indication: Paracetamol poisoning
Mode of Action: Protects against liver and renal toxicity in cases of paracetamol poisoning. It acts as a precursor of glutathione to replenish gluthione stores in the liver cells.
Dosage: 2-5 grams followed by three 2.5 grams doses every 4 hours.
Naloxone
Indication: Opioid overdose
Mode of Action: A specific opioid antagonist that acts directly at opioid receptors to inhibit its toxicity effects.
Dosage: 0.4 mg through intravenous push as initial dose which can be further repeated every 2-3 minutes to a maximum bolus of 2 mg.
Penicillamine
Indication: Lead, copper and arsenic poisoning
Mode of Action: Binds with heavy metals to form stable water-soluble complexes that can be excreted in the urine.
Dosage: Total of 1-2grams daily in divided doses throughout the day.
Phentolamine
Indication: Alpha-adrenergic poisoning, cocaine toxicity
Mode of Action: Blocks alpha1 adrenoreceptors to inhibit vasoconstriction and decrease peripheral resistance thereby reducing blood pressure. For cocaine toxicity, it acts as an alpha-blocker to reduce cocaine-induced coronary vasoconstriction thereby resolving cocaine-induced myocardial ischemia.
Dosage: 2.5mg IV bolus and maybe repeated if necessary.
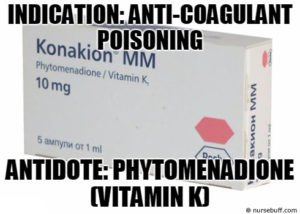
Phytomenadione (Vitamin K)
Indication: Anti-coagulant poisoning
Mode of Action: Interrupts anti-coagulant’s antagonistic effects on vitamin-dependent coagulation factors thereby reducing anti-coagulant poisoning effects.
Dosage: 10-20mg orally
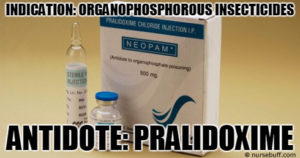
Pralidoxime
Indication: Organophosphorous insecticides
Mode of Action: Restores acetylcholinesterase activity by removing phosphate compounds in the phosphorylated acetylcholinesterase to reestablish normal acetylcholinesterase activities.
Dosage: 30mg/kg through intravenous for five to ten minutes and may be repeated at 4-6 hour intervals.
Procyclidine
Indication: Induced dystonia caused by anti-psychotic drugs and metoclopramide
Mode of Action: Elicits anti-muscarinic actions to relieve parkinsonian symptoms caused by antipsychotic drugs and metoclopramide
Dosage: 5-10mg through oral, IV or IM routes. Additional oral doses may be required for 2-3 days.
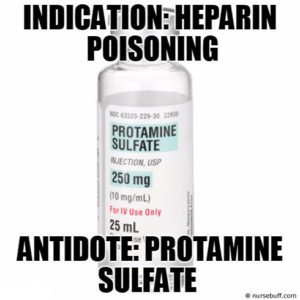
Protamine sulfate
Indication: Heparin poisoning
Mode of Action: Binds with heparin to neutralize anti-coagulative effects in the bloodstream.
Dosage: Maximum of 50mg dosage in a ten-minute period.
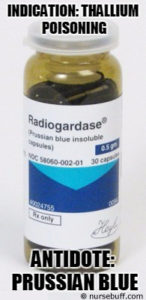
Prussian blue
Indication: Thallium poisoning
Mode of Action: Mobilizes intracellular thallium by absorbing thallium into the insoluble crystal lattice of Prussian blue in the gastrointestinal tract.
Dosage: 250mg/kg per day orally in divided doses administered through a nasogastric tube
Silibinin
Indication: Amatoxin poisoning
Mode of Action: Protects the liver by blocking entry of amatoxins into the hepatic cells.
Dosage: 20mg/kg daily divided into 4 infusions with each infusion running on two-hour duration
Sodium Calcium Edetate
Indication: Lead toxicity
Mode of Action: Binds with divalent and trivalent metals like lead to form water soluble ring-compound to be readily excreted in the urine.
Dosage: 30-40 mg/kg through intravenous infusion either in 5% Dextrose or 0.9% saline twice daily for up to 5 days.
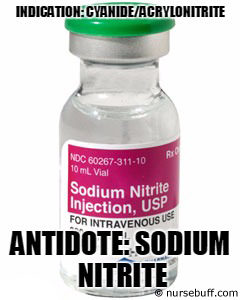
Sodium nitrite
Indication: Cyanide/acrylonitrite
Mode of Action: Nitrites facilitate conversion of hemoglobin to methemoglobin. Methemoglobin has higher binding affinity to cyanide which further facilitates its excretion.
Dosage: 10mL of 3% sodium nitrite solution through IV for 5-20 minutes followed by sodium thiosulphate
Sodium thiosulphate
Indication: Cyanide/acrylonitrite
Mode of Action: Acts as a precursor for the enzyme rhodanase which facilitates conversion of cyanide to non-toxic thiocyanate and thereby promoting its excretion.
Dosage: 50mL of 25% sodium thiosulphate through IV for ten minutes
Starch
Indication: Iodine
Mode of Action: Converts iodine to iodide which is less harmful.
Dosage: 15gram starch in 500 mL water orally
Also Read: Laboratory Values and Interpretation: A Nurse’s Ultimate Guide
Tips in Starting a Poison Control Center
A Poison Control Center is a medical facility that provides immediate free first aid and treatment advice for poisonings over a telephone call. This center is composed of doctors, nurses, pharmacists and other professionals who are experts in poison treatment and control. It is open 24 hours a day and accessible to everyone through a phone call.
If you want to help in establishing a Poison Control Center in your area, take note of the following tips:
1. The Poison Control Center Staff must be trained in the field of Toxicology.
2. Staff should have proper phone etiquette skills. They will be dealing with emergency poisoning situations in the home. For this reason, the staff on duty should maintain his presence of mind in giving first aid advices amidst panicked calls of poisoning.
3. The Poison Control Staff should follow up referrals to ERs. There are cases of poisoning that cannot be treated at home and need to be managed in the ER. The PC staff is responsible in ensuring that referred patients successfully reach the referred ER department.
4. The Poison Control Center 24-hour hotline should have TYY/TDD number for hearing-impaired callers.
5. Always be updated with the National Poison Data System as released by the American Association of Poison Control Centers.
With these basic facts about common drugs and their antidotes, you are now armed with valuable knowledge about managing cases of poisoning in your areas. Always keep yourself updated with the latest toxicology news and reports as poison management is an ever-changing field in medicine.
Also Read: Emergency First Aid for Nurses: A Practical Guide