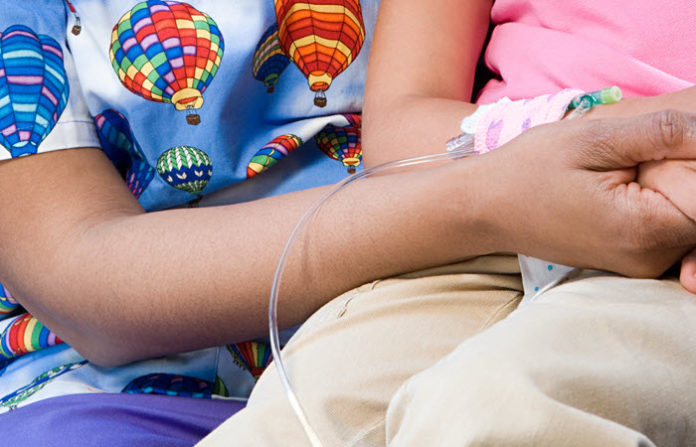
Performing IV insertion on pediatric patients is undeniably one of the most daunting tasks for nurses. It’s also possibly one of the most traumatic experiences among young patients.
As much as nurses want to turn this painful experience into a memorable role-playing game, the mere sight of needles and nurses in white uniforms are enough to scare the hell out of these young patients.
In addition to their developmental limitations, pediatric patients also pose additional challenges for the nurse/IV therapist, just like in the case of patients with fragile veins or edematous tissues. Plus, with work overload and having less time, a lot of nurses and healthcare providers fail to use comforting strategies (1) to help their pediatric patients.
A painless venipuncture is almost impossible to achieve but that doesn’t mean that you can’t do it safely and properly.
Here are 10 of the most effective ways to make IV insertion in pediatric patients less stressful.
1Determine the child’s developmental stage
Every child achieves a particular developmental milestone for every age range. Hence, a nurse should take into consideration the child’s developmental age. This will determine the correct IV insertion site, the size of the catheter to be used as well as the manner on how health information or instruction will be disclosed.
2Perform venipuncture in a neutral place
For a child, the hospital room is his “safe haven” and doing a painful procedure within this place is tantamount to trespassing into his own little world.
Every patient has his or her own special needs. In the case of young patients, respect should be put in high regard. As a rule, painful procedures must be done outside of the patient’s room or in a specific treatment room assigned for this purpose.
3Avoid applying restraints as much as possible
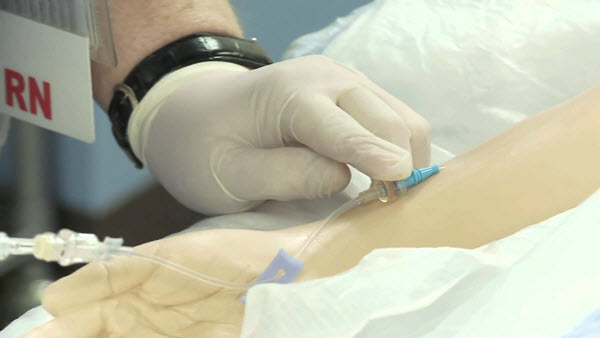
IV insertion is a traumatizing experience in itself so restraining the child during this procedure will only put the patient’s psychological development in peril.
For this reason, using strict restraining procedures to control the patient’s bodily movements should not be allowed. If it is considered necessary, using less invasive restraining procedures like the “hug technique” with the help of the parents will provide more warmth and additional emotional support to the young patient.
4Use creative forms of distraction
There are a variety of ways a nurse can distract a child who is about to undergo IV insertion.
According to experts, letting the patient blow bubbles, sing or count as the IV insertion procedure progresses have been found effective, especially for preschool or school-age children. In the U.S., the use of iPads as a distraction tool has gained a lot of praise from nurses around the country. As a matter of fact, in 2009, Child Life Services began using two iPads in a trial run (2). The computers are now used by the department for:
- Preparation: Patients and families learn online about the procedure to come. They can reference a pictorial roster of child life specialists to familiarize themselves with a new face if they’re about to go to a new unit.
- Distraction: The patient can play games on the computer during an IV insertion.
- Education: The Child Life specialist can help access customized diagnosis information for the patient and family.
5Use a tourniquet appropriate for the size of your patient
Dilating the veins of a pediatric patient might become an overwhelming task for any nurse but Nurse Ann Marie Frey has given the following advice:
To dilate veins in children, use a tourniquet appropriate for the size of your patient and position it several inches above the intended site. To place a device in a scalp vein, a rubber band with a tape tab, placed above the eyes and ears, is an easily removable tourniquet. Make sure the tourniquet isn’t too tight or on too long, indicated by red or purplish skin. You should be able to distend veins but still feel a pulse.
To ease the discomfort of the tourniquet, you can tie it over a sleeve or a gauze 4×4. In some cases, especially with premature neonates, you’ll be able to see or feel veins well enough to access them without using a tourniquet.
6Choose age-appropriate IV sites
Choosing the best site for IV insertion among pediatric patients can be a lot more taxing than the actual insertion procedure. Here are some important reminders to do it successfully:
- Scalp veins are easy to access and most appropriate in neonates; an older infant might dislodge a device placed there.
- Hand and foot veins are appropriate for children of all ages, but try to use foot veins only in children who aren’t walking yet. If possible, try not to choose a vein in a child’s dominant hand or the hand she favors for thumb sucking.
- Digital veins are useful in toddlers and older children if other sites aren’t accessible, but they infiltrate easily because the site is difficult to immobilize in an active child.
- The forearm or upper arm is suitable for all children, but veins there may be harder to access, especially in infants and toddlers, where veins may hide under subcutaneous fat. Arm sites allow for larger-sized catheters and hand mobility.
- Antecubital sites (cephalic, basilic, or median cubital vein) are suitable for all children and are easy to locate in infants. But these sites are uncomfortable and require immobilizing the elbow. Because this site is also used for phlebotomy and peripherally inserted central catheter placement, it shouldn’t be your first choice.
7Let the parents be with their child

For some young patients–especially those who are 7 years old and below–the presence of a parent can significantly reduce their anxiety. Older children should also have the option to let their parents be on their side during the procedure to provide additional support. For this reason, nurses should never disregard the parent’s participation in this painful procedure.
8Don’t give false expectations
Proving false assurance is never considered a therapeutic communication technique for psychiatric patients and the same goes for pediatric patients who are about to undergo IV insertion. It’s not even considered a good bedside manner for nurses.
The younger the child, the less amount of information you have to give immediately before the procedure. Never tell a young patient that venipuncture won’t hurt or it will only take 2 seconds to complete when it’s actually not. Be honest and try to use a logical way to set the patient’s expectations.
9Choose the smallest gauge catheter
According to expert nurse practitioners, a nurse should choose the smallest-gauge catheter (24 or 22) in the shortest length to allow hemodilution of infusates by blood flow around the catheter. In neonates, administer I.V. fluids and medications, blood, and blood products via a 24-gauge I.V. device. In older children, a 24- or 22-gauge catheter works without increasing the risk of hemolysis.
10Protect the IV site to prevent dislodgement
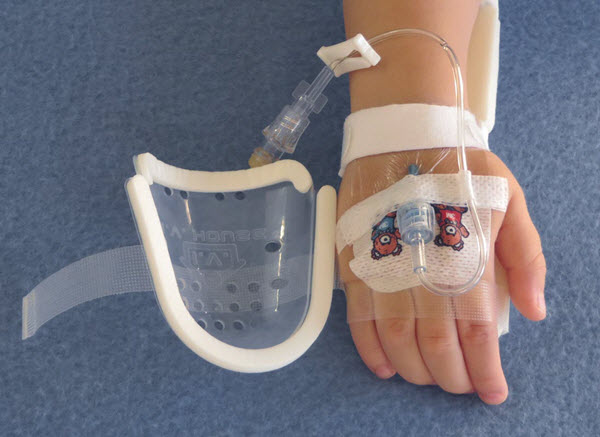
Pediatric patients are naturally curious and active even during times of hospitalization, further increasing the chances for the IV tubes to be dislodged from the veins. This is the reason why transparent protective devices or stockinette bandages are being advised to be used for this particular group of patients. If the IV insertion site is near a joint, use of arm board with adequate pads are also recommended.
See Also: 8 Nursing Lifehacks in Caring for Pediatric Patients
IV insertion in pediatric patients can be quite challenging especially for new nurses but with the right practice and with the use of the 10 tips mentioned above, mastery of this procedure will never be out of reach anymore. Nursing is an art so we have to strive further to make every nursing procedure a pleasant experience for both the nurses and the patients that we care for.
To get a clearer idea, you can watch this step-by-step guide:
Check Out Our Infographic

Share this Image On Your Site
References:
1. Katende, G., & Mugabi, B. (2015). Comforting strategies and perceived barriers to pediatric pain management during IV line insertion procedure in Uganda’s national referral hospital: A descriptive study. BMC pediatrics, 15(1), 122.
2. Burns-Nader, S., Atencio, S., & Chavez, M. (2016). Computer tablet distraction in children receiving an injection. Pain Medicine, 17(3), 590-595.