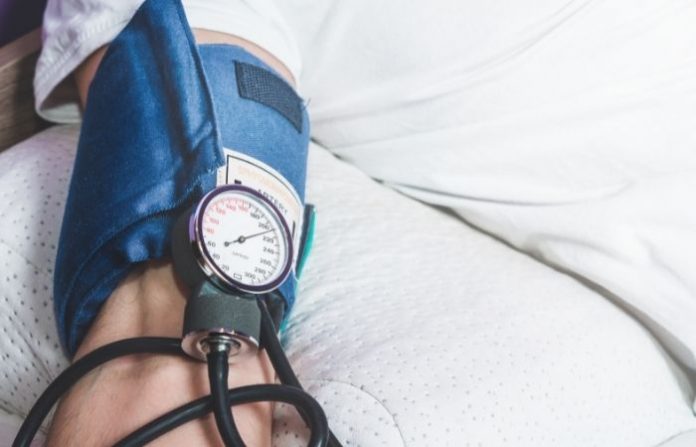
As nurses, we all know that hypertension or prolonged elevation of blood pressure can be considered a medical emergency if not adequately managed. But in reality, not all patients admitted in E.R. are considered “emergency cases”. After careful evaluation, some are discharged, sent home, and given follow-up instructions.
Severely elevated blood pressure is defined as systolic blood pressure of 180 mm Hg or greater and diastolic blood pressure of 110 mm Hg or greater. If improperly controlled, it could lead to various organ dysfunctions or even death.
But the question is: when it is an emergency?
Severely elevated blood pressure or SEBP may be stratified into 3 categories:
1. Hypertensive Emergency
Hypertensive emergency is described as severe elevations in BP (>180/120 mm Hg) complicated by evidence of impending or progressive target organ dysfunction. Symptoms and signs can point to adverse effects of SEBP on target organs, often called target-organ dysfunction/damage or end-organ damage. The organs most likely to be affected by hypertension include the heart, brain, kidneys, and eyes.
Signs and symptoms:
- chest pain
- shortness of breath
- cough
- orthopnea
- palpitations
- weakness or fatigue
- dizziness
- nausea
- other symptoms of ischemic heart disease
- headache
- vomiting
- seizures
- acute confusion
- stupor
- coma
Hypertensive emergency can also lead to stroke with signs and symptoms of headache, dizziness, lightheadedness, vertigo, tinnitus, visual changes, mental status changes or confusion, weakness, hemiplegia, ataxia, speech alterations, and other neurological deficits. Blurred vision or transient blindness, hematuria, oliguria, and anuria may also be present.
Patients with signs and symptoms of aortic dissection may present with the following:
- chest, abdominal, or back pain
- back or flank ecchymosis or Grey Turner sign
- unequal or absent pulses in the extremities
- signs and symptoms of shock including hypotension, tachycardia, pale clammy skin, decreased urine output, altered level of consciousness
Patients with abdominal tenderness on palpation should be seen immediately by a medical practitioner. Such case is considered critical.
2. Hypertensive Urgency
Patients under hypertensive urgency may present, often to the emergency department, with signs and symptoms that require provider attention but are not an emergency. Also included are those situations associated with severe elevations in BP without progressive target organ dysfunction.
Examples include upper levels of stage 2 hypertension associated with severe headache, shortness of breath, epistaxis, or severe anxiety. Patients with these signs and symptoms are usually known as hypertensive patients who have been non-compliant with their medication regimen or have blood pressure that has not been adequately treated.
3. Severe Asymptomatic Hypertension

Severe asymptomatic hypertension is defined as hypertension present but without signs or symptoms of acute end-organ damage.
Patients often present to the emergency department or urgent care or primary care clinic for a problem unrelated to blood pressure but are found to have SEBP.
Important Reminders for Nurses and Health Care Providers:
- Lowering blood pressure too aggressively on patients with hypertensive emergency may even precipitate a stroke.
- Actual level of elevation or absolute level of blood pressure may not be as important as how quickly the blood pressure rises. An abrupt, severe rise in blood pressure is an important indicator in determining the need for emergency treatment.
- Normotensive individuals with normal vasculature are more sensitive to sudden elevations in blood pressure and may develop end-organ damage at lower blood pressure levels. As a result, care cannot be based solely on the level of blood pressure elevation.
- The nurse should ask whether the patient has high blood pressure/hypertension and if there is a history of angina, acute myocardial infarction, transient ischemic attack or stroke, kidney disease, or retinal problems.
- In addition to a careful history, a detailed review of medications is essential. Thus, it is important to determine what medication the patient was taking, how long medication has been stopped, or when the patient took the last dose of antihypertensive medication.
- Hypertensive emergency can be encountered in any type of surgical procedure but happens more often in cardiothoracic surgery, vascular surgeries such as endarterectomy and aortic repairs, neurosurgery, head and neck surgery, and renal transplantation.
- Hypertensive emergency occurs most commonly in patients with a known history of hypertension who have not been compliant with medication therapy, have run out of or stopped medication, or whose blood pressure is not controlled with medication.
In general, updating our knowledge with recent research studies will make us more competent and confident in the care we provide to our patients. Hypertension should never be taken for granted because the result of that neglect might be a long-term disability or even death. Prevention, through immediate medical attention and health teachings, will always be better than cure.