In the world of medicine, two terms often surface in conversations about life-threatening situations: clinical death and brain death. While both these terminologies encompass the idea of death, they represent different stages in the dying process.
As a nurse, it’s crucial to get a really good understanding of these stages. This article examines each one’s features and explores their temporal relationship so you can have a better idea of which stage really comes first.
Clinical Death: The Early Stage
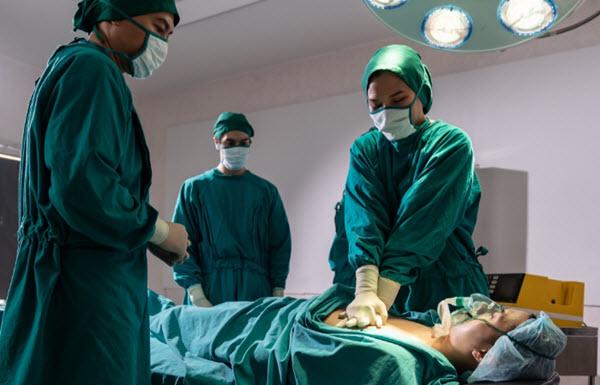
Clinical death, the earlier stage of the two, is characterized by the cessation of vital signs such as heartbeat and respiration. It signifies the moment the heart stops beating, causing blood circulation to halt.
Despite its ominous nature, clinical death is considered a reversible state, thanks to modern medical interventions. The reason for its reversibility lies in the resilience of our body’s cells, particularly those in the brain. They can remain viable for several minutes after blood flow ceases.
For instance, in situations like cardiac arrest, prompt cardiopulmonary resuscitation (CPR) can restore circulation, effectively reversing clinical death. This state and its potential for reversal underline the vital importance of immediate medical response in life-threatening scenarios.
Brain Death: The Point of No Return
In contrast, brain death signifies an irreversible end-point. It occurs when there is a complete and permanent cessation of all brain functions, including in the brainstem.
A person declared brain dead is legally and medically recognized as deceased, even if other physiological processes can be artificially maintained.
The confirmation of brain death is based on comprehensive clinical examinations and the absence of specific reflexes. Updated criteria from the American Academy of Neurology in 2020 also mandate the use of confirmatory tests like electroencephalography (EEG) or cerebral angiography, which track brain activity or blood flow, respectively.
The Nurse’s Role: Navigating Clinical and Brain Death

Nurses play a crucial role in managing and supporting patients during the stages of clinical death and brain death, offering both medical and emotional support to patients and their families.
During a clinical death situation, such as cardiac arrest, the first-line intervention usually involves immediate resuscitation attempts. Nurses are often the first responders, performing CPR and using automated external defibrillators (AEDs) to attempt to restore cardiac function and blood circulation.
Along with these urgent medical responses, nurses must maintain clear communication with the entire medical team, swiftly and accurately sharing patient information. They monitor and report any changes in patient status, contributing vital information that helps to shape the course of ongoing resuscitation efforts.
The nurse’s role takes a dramatic turn when facing potential brain death. Nurses must understand the intricacies of brain death diagnosis, including the observational and confirmatory tests. While physicians ultimately confirm brain death, nurses’ consistent monitoring and data collection can guide this process.
Once brain death is confirmed, a nurse’s responsibilities evolve from medical care to providing emotional support for the bereaved family. Nurses play a pivotal role in offering comfort, explaining the circumstances, and guiding the family through their grief and the subsequent decisions that must be made, such as organ donation.
In both clinical and brain death scenarios, nurses represent the intersection of medical expertise and compassionate care. They ensure the best possible care for patients, even in the face of death, while also offering vital support to families during these most challenging moments. The role of a nurse is thus a testament to the deeply human side of healthcare, emphasizing empathy and understanding in tandem with medical skill.
Essential Reminders for Nurses Navigating Clinical and Brain Death
Nurses play a critical role in managing and supporting patients and their families through the stages of clinical death and brain death. Here are some key points to remember:
Be Prepared: Familiarize yourself with the resuscitation protocols, procedures, and equipment in your healthcare setting. In times of crisis, every second counts.
Communicate Effectively: Ensure clear, precise, and immediate communication with the entire medical team during resuscitation efforts. Documentation should be accurate and up-to-date.
Understand the Indicators: Know the signs of clinical death and brain death. Accurate observation and assessment are critical in these situations, and your insights can guide further medical intervention.
Stay Informed: Keep up-to-date with the latest research and developments in resuscitation and brain death management. The more informed you are, the better positioned you will be to offer quality care to your patients.
Offer Emotional Support: The transition from clinical death to brain death is a traumatic experience for families. As a nurse, you play a pivotal role in offering emotional support, explaining the situation, and guiding them through their grief.
Know the Ethical Guidelines: Familiarize yourself with the ethical guidelines related to end-of-life care and organ donation.
Practice Self-Care: Dealing with death is emotionally challenging. Make sure to look after your own mental and emotional health, seeking support when needed.
Remember, your role as a nurse extends beyond medical care. It involves compassionate communication, ethical decision-making, and emotional support. By keeping these points in mind, you can navigate the complexities of clinical death and brain death, providing comprehensive care to your patients and their families.
Final Thoughts: Weaving Threads of Life and Death
Nurses play an irreplaceable role in these intense transitions. Their unique blend of clinical expertise and empathetic support provides a critical lifeline for patients and families alike, helping them navigate the emotional turbulence that often accompanies these stages.
As a nurse, our understanding of these stages should broaden not just our medical horizons but also our understanding of life’s inherent value.