This February, the Centers for Disease Control and Prevention (CDC) released the new Adult Immunization Schedule for 2017. It consisted of important changes in recommendations for adult vaccination schedules as approved by the Advisory Committee on Immunization Practices (ACIP).
While children are required to complete the recommended immunizations for them so they can attend public school, immunizations for adults are not compulsory. However, clinicians strongly suggest compliance to recommended immunizations for added protection against vaccine-preventable diseases especially among high-risk groups.
Why is it important for nurses?
Nurses are usually the first point-of-contact of patients seeking information about immunizations.
Vaccine formulations and preparations change rapidly over the years. To cope with the frequent changes, advisory committees regularly update immunization recommendations so they can ensure vaccines’ safety and efficiency for the general public. Nurses, like other healthcare professionals, should be champions in educating patients about their options in immunization.
Also, there are special vaccine recommendations for patients with existing comorbidities. Nurses should be aware of this information so they can properly educate their patients when providing nursing care to them.
2017 Adult Immunization Schedule Changes
The major changes in the recommended Adult Immunization Schedule affected four types of vaccines – influenza, human papilloma virus (HPV), meningococcal and hepatitis B vaccines.
Influenza Vaccine
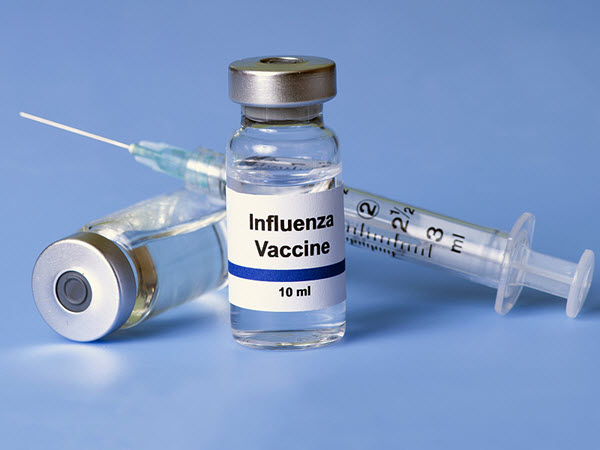
The changes in recommendations for Influenza immunization are based on the vaccine’s documented effectiveness during the 2013-2014 and 2015-2016 flu seasons. Recommendations for people with egg allergies, who were contraindicated with influenza vaccine in the past, are also updated.
- Live Attenuated Influenza Vaccine (LAIV) available in nasal spray preparations under the brand names FluMist and MedImmune is no longer recommended for the 2016-2017 flu season.
- Adults with a history of egg allergy can now receive Inactivated Influenza Vaccine (IIV) or Recombinant Influenza Vaccine (RIV) as long as their known allergic reaction to eggs is limited to hives only.
- Adults with a history of egg allergy who had more severe allergy symptoms like dyspnea, lightheadedness, emesis or angioedema that required emergency medical attention can still receive IIV or RIV. However, the vaccine should be administered in an in-patient or out-patient clinical setting under the supervision of a healthcare professional. This is required so the healthcare professional can monitor and manage the development of severe allergic reactions after the administration of the vaccine.
Human Papillomavirus (HPV) Vaccine
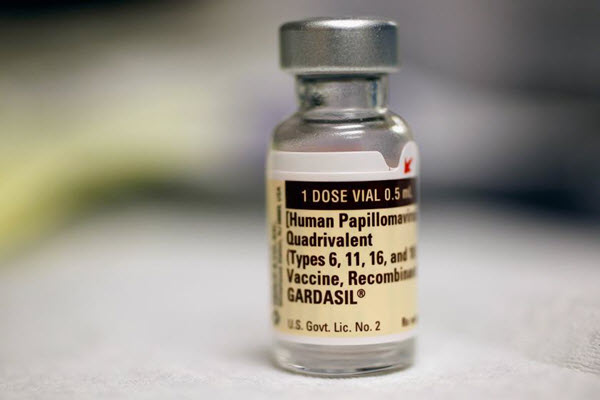
Human Papillomavirus (HPV) Vaccine has been recommended to be started before the age of 15 among adolescents in a 2-dose, 5-month apart schedule. Those who did not start HPV immunization before the age of 15 are recommended to receive 3 doses of the vaccine. More detailed recommendations were released about these existing guidelines.
- For those who have no history of HPV vaccine: Women through age 26 years and men through age 21 years should receive 3-dose series of HPV vaccine at 0, 1st-2nd, and 6th month schedule. Men aging 22 through 26 years may still be vaccinated with the same 3-dose series of HPV vaccine.
- For those who completed 2 doses of HPV vaccine at least 5 months apart before the age of 15: They are considered adequately vaccinated and have no need for an additional dose of HPV vaccine.
- For those who received only 1 dose or 2 doses of HPV vaccine less than 5 months apart before the age of 15: Women through age 26 years and men through age 21 years should receive 1 additional dose of HPV vaccine. Men aging 22 through 26 years may also be vaccinated with 1 additional dose of HPV vaccine.
Meningococcal Vaccine
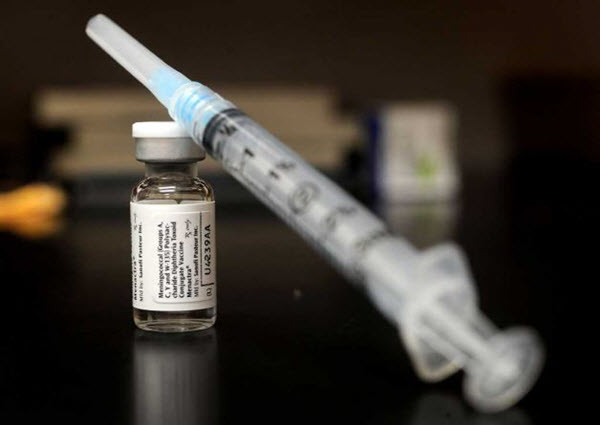
There are two groups of meningococcal vaccines – the Serogroup A, C, W, and Y Meningococcal Conjugate Vaccine (MenACWY) and the Serogroup B Meningococcal Vaccines (MenB) (MenB-FHbp [Trumenba, Pfizer]).
- Adults with HIV infection who never received Meningococcal Vaccine before should receive 2-dose MenACWY series. It should be given at least 2 months apart and should be revaccinated every 5 years. Those who received 1 dose of MenACWY vaccine before can proceed with their 2nd dose, administered at least 2 months after the 1st dose. Immunization with Serogroup B Meningococcal Vaccines is not routinely recommended as meningococcal infection among adults with HIV infection is primarily caused by serogroups C, W, and Y only.
- Adults with functional or anatomical asplenia or persistent complement component deficiencies should receive 2-dose MenACWY series. It should be given at least 2 months apart and should be revaccinated every 5 years. They should also receive Serogroup B Meningococcal Vaccines with either MenB-4C in 2-dose schedule at least 1 month apart or MenB-FHbp in 3-dose schedule at 0, 1st-2nd, and 6th month.
- During a meningococcal disease outbreak, adults at risk should receive 1 dose of MenACWY if the outbreak is related to Serogroup A, C, W, or Y. If the outbreak is related to Serogroup B strains, adults at risk should be vaccinated with either MenB-4C in 2-dose schedule at least 1 month apart or MenB-FHbp in 3-dose schedule at 0, 1st-2nd, and 6th month.
- Microbiologists working on or routinely exposed to isolates of Neisseria meningitidis should receive 1 dose of MenACWY and be revaccinated every 5 years. They should also receive either MenB-4C in 2-dose schedule at least 1 month apart or MenB-FHbp in 3-dose schedule at 0, 1st-2nd, and 6th month.
- Young healthy adults aging 16 through 23 years who are not at increased risk for Serogroup B Meningococcal Disease may receive either MenB-4C in 2-dose schedule at least 1 month apart or MenB-FHbp in 3-dose schedule at 0, 1st-2nd, and 6th month for short-term protection against Serogroup B Meningococcal strains.
- Adults who are at increased risk for meningococcal disease and those who were immunized during Serogroup B Meningococcal disease outbreaks should receive MenB-FHbp in 3-dose schedule at 0, 1st-2nd, and 6th month.
- If MenB-FHbp is given to healthy adolescents and young adults who are not at increased risk for meningococcal disease, 2 doses of MenB-FHbp should be given at 0 and 6 months.
Hepatitis B Vaccine
Hepatitis B immunization is recommended to people suffering from chronic liver disease conditions because they are at high risk for hepatitis B infection. ACIP introduced updates to these conditions.
– Adults with the following chronic liver conditions should receive Hepatitis B vaccine series:
o Hepatitis C infection
o Fatty liver disease
o Liver cirrhosis
o Autoimmune hepatitis
o Alcoholic liver disease
o Alanine aminotransferase (ALT) levels greater than twice the upper limit of normal
o Aspartate aminotransferase (AST) levels greater than twice the upper limit of normal
More detailed information about the 2017 Adult Immunization Schedule can be found HERE while you can get the code for immunization schedules for your website HERE.
With these changes, researchers are expecting that more adults can now benefit from the recommended immunization schedules. However, it will take time before you can memorize the changes in the recommended guidelines. If possible, bring an Immunization Schedule Chart when discussing it with your patient to provide them with complete up-to-date information about their options.
See Also: 7 Vintage Medical Equipment Nurses Used in the Past