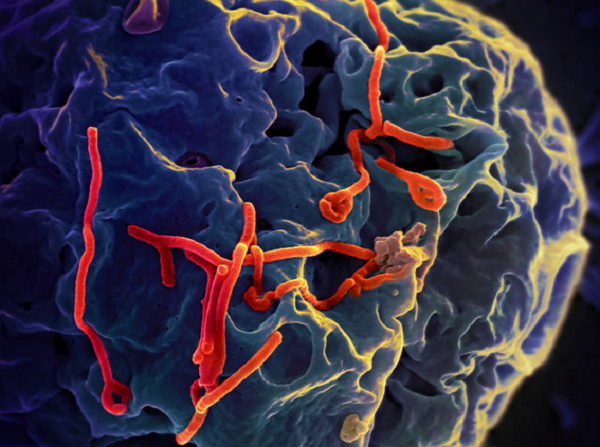
The Ebola Virus Disease is now a major epidemic affecting most parts of West Africa, and is beginning to invade other countries as well.
In the past decades, this disease was just known for small outbreaks in remote areas of Democratic Republic of Congo. Sporadic outbreaks after the 1976 discovery of the virus had been quickly controlled, although cases were usually fatal.
Now that the disease has gained its momentum in spreading across different nations, are you prepared to face it as a nurse?
1. What Is Ebola Virus Disease?
The Ebola Virus Disease is a hemorrhagic viral disease caused by the infection of one of the Ebola strains.
Currently, there are five Ebola virus strains, four of which are infectious to humans – Ebola virus (Zaire ebolavirus), Sudan virus (Sudan ebolavirus), Bundibugyo virus (Bundibugyo ebolavirus) and Taï Forest virus (Taï Forest ebolavirus, formerly Côte d’Ivoire ebolavirus).
The fifth one is Reston virus (Reston ebolavirus) and it is only known infectious among non-human primates. It is long-believed that the Ebola viruses are animal-borne and their main reservoirs are bats.
2. Ebola Virus Origin.
Ebola was first discovered in 1976 after mysterious hemorrhagic outbreaks happened in Sudan and Zaire. The virus was named after the Ebola River in Zaire which is now part of the Democratic Republic of Congo.
Scientists from Belgium first isolated the virus from a blood sample of a Belgian nun who died in Zaire. The disease was first transmitted through close contact with infected individuals and reuse of contaminated needles and syringes.
3. How Is Ebola Transmitted?
Ebola is transmitted through direct contact with blood and body fluids of infected individuals. Once a person is infected with the virus, he or she should show signs and symptoms of the disease in order to be infectious to others.
The excreted body fluids that contain Ebola viruses are urine, vomitus, feces, sweat, tears, mucus, phlegm, saliva, semen and breast milk.
Direct contact with the infected individual’s personal belongings has also been known to cause the transmission of infection. The Ebola virus disease is highly infectious and incubation period is usually 2-21 days.
4. Signs and Symptoms.
The signs and symptoms of the Ebola Virus Disease are similar to other hemorrhagic viral diseases.
It starts with fever, vomiting, diarrhea, muscle pain, weakness, severe headache and unexplained hemorrhage. They will appear 2 to 21 days after exposure but the average for most patients is 8 to 10 days.
Once the disease has progressed, internal and external hemorrhage will occur which makes it fatal in most cases. Laboratory examinations commonly show low white blood cell and platelet count as well as elevated liver enzymes.
5. Treatment and Management.
Treatment of Ebola Virus Disease is supportive in nature. The symptoms are treated as they appear.
Nursing management includes providing IV fluids to maintain hydration and electrolyte balance, maintaining blood pressure, and supporting oxygen status.
There is no known effective medication for the disease although experimental drugs and vaccines are already underway. Because the disease is characterized by fluid loss and hemorrhage, it is highly contagious among healthcare workers.
With insufficient knowledge about its transmission along with improper wearing of PPE, nurses have the greatest chance of being infected.
6. Infection Prevention.
Once the Ebola Virus Disease is suspected or confirmed, nurses should institute standard, droplet and contact precaution.
The patient should be placed in a single room with its own bathroom. The door to hallways should always be closed. Wear personal protective equipment (PPE) before patient contact. It includes:
- Fluid-resistant or impermeable gown with hood
- Goggles or eye shield
- Facemask
- Gloves
If you will be likely exposed to blood and body fluids, additional PPE should be worn:
- Double gloving
- Disposable shoe covers
- Disposable leg covers
When wearing and removing PPE, it is best to use the buddy system to ensure fit and safety. Remove the PPE carefully without contaminating your eyes, mucous membranes and skin. Discard the PPE properly and do hand hygiene immediately afterwards.
7. Patient Care Considerations.
When dealing with a confirmed case of Ebola infection, all persons entering the rooms should be recorded and monitored in the next 21 days for possibility of cross infection.
Limit the use of needles and other sharps whenever possible. Limit contact with the infected patient as much as possible; plan and group your tasks when entering the patient’s room so you can do them all at once.
When assessing the patient, always check for tendencies of bleeding and ensure that there is proper fluid balance in the patient’s body.
8. Tips In Dealing With A Suspected/Confirmed Ebola Case:
- When assessing a patient in the triage area, those with reports of fever starting at ≥100.4°F / 38.0°C along with other compatible symptoms of Ebola Virus Disease (EVD) and a history of travel to Ebola-hit areas in the last 21 days should be suspected of infection. In general, there are three keys in suspecting Ebola infection – 1. Fever, 2. Occurrence of other EVD symptoms and 3. Known exposure to an Ebola case or recent travel to Ebola-hit areas in the past 21 days. Report it immediately and create a record of people that have been in contact with the suspected case in the triage area.
- When doing aerosol-generating procedures to an Ebola patient, institute airborne precaution. Wear additional PPE like N95 and limit the presence of personnel in the patient’s room.
- Keep in mind that the likelihood of Ebola infection among nurses and other healthcare workers is high because of holes in donning and removing PPE. Always have presence of mind and be strict with yourself when donning and removing PPE using the buddy system.
- Handle body wastes with extra care. There are high concentrations of Ebola viruses in urine, vomitus, feces, sweat and other body fluids.
- The transmission of Ebola infection is also known to be caused by direct contact with the things the patient used so you should always follow proper disinfection protocols for reusable items in patient care.
- In assessing and evaluating patient’s condition, remember that the major symptom of this disease is fluid loss. Look for complications that severe fluid loss may cause like hypotension, electrolyte imbalance, dehydration, coagulation problems and organ failure.
- Always practice hand hygiene. The transmission of Ebola infection is fast but doing proper hand hygiene before and after patient care will decrease the likelihood of cross infection.
Now, are you ready to face the battle against Ebola?
Our healthcare system is in the phase of developing and improving Ebola handling protocols, but it is best to know the basics of handling this infectious disease.
Additional Resources:
1. Ebola Hemorrhagic Fever – Centers for Disease Control and Prevention (CDC)
3. Ebola: what nursing staff need to know
About the Author: Je Abarra is a nurse by profession and a freelance writer by passion. She is working as a staff nurse in the pediatric ward of a private city hospital for more than two years. During her free time, she usually writes about her fascinations in health and nursing. She loves to provide tips and fun facts about nursing and healthy living.