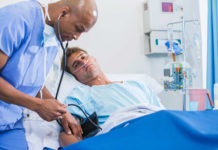
People, how is your nurse bedside manner?
A good nurse-client relationship is essential in ensuring quality patient care. Therapeutic communication is the key to achieving this and a nurse’s soft skills are important in making it possible.
Although the patient’s sociocultural and psychological well-being are critical considerations in proper bedside manner, there are helpful conversation hints that will guide you in responding correctly to your patients.
Here are some tips in achieving better bedside manners:

Don’t: Talk rapidly, ask multiple sets of questions or change subjects rapidly.
Why: Patients can get easily confused. They might not be able to communicate effectively.Example: “What is your name? I see you like books. How do you feel?”
Do: Give broad openings so you can have clues on what to explore with your patient.
Example: “Hi I’m Lina, your nurse. What do you want to talk about for today?”
![]()
Don’t: Give your own judgment, opinion or beliefs. Using words like “great, nice, wrong, bad, good, should, ought, etc.” implies judgment.
Why: This is a common source of misunderstandings between a nurse and a patient. A patient may fear communicating his thoughts with a nurse who is openly vocal about opinions or judgments.
Example: “That’s wrong. You shouldn’t think of that. As a Christian, we should not be initiators of such thoughts.”
Do: State to the patients what you have observed so they can validate that you understood their statements. Summarize by reviewing the main points of your discussion.
Example: “You sound worried. At the beginning, you stated that you doubt your decisions and that includes…”
![]()
Don’t: Fail to give feedback, be inappropriately unresponsive
Why: A patient’s statements should not be taken for granted. They need to be acknowledged as they might contain important cues that may reflect the patient’s condition.
Example: The patient asked the nurse about his diet but she walked away.
Do: Practice active listening. Observe for both verbal and non-verbal cues from the patient. Maintain eye contact and make verbal remarks to encourage progression of communication.
Example: “Yes I heard you. You were prescribed a low salt and low-fat diet. You can have lean meat and vegetable for your meals. Are you having trouble in choosing what to eat?”
![]()
Don’t: Give false reassurance or unrealistic expectations like using clichés to allay your patients’ worries or fears.
Why: Patients may lose their trust on their healthcare team if the false reassurance they heard turned out to be impossible.
Example: “Don’t worry about your diagnosis. Everything’s going to be alright.”
Do: Set realistic expectations. Give information that will help the patient better understand the situation.
Example: “You are diagnosed with Acute Lymphoblastic Leukemia. There are treatments for it like chemotherapy and radiotherapy.
See Also: 4 Most Important Tips on Caring for Child Cancer Patients
![]()
Don’t: Ask “why” directly to the patient.
Why: Asking the question “why” may result in a negative impact. It will make him feel judged which may lead to defensive answers.
Example: “You said you think the doctor has a wrong diagnosis. Why?”
Do: Explore the patient’s statement and be objective in asking follow-up questions. You can still get to the reason behind the patient’s statement by changing your approach.
Example: “You said you think the doctor has a wrong diagnosis. Is there other information or symptoms you want to share?”
![]()
Don’t: Express your feelings or any personal details.
Why: When establishing rapport, your feelings or any personal details are irrelevant to the patient. Talking more about yourself will spoil the budding rapport you are establishing with your patient.
Example: “Do you like the flowers here in your room? I like them, in fact, my garden back home is full of different flowers.”
Do: When talking with your patient, keep in mind that the conversation should be about him. This way, he can feel that you are a good listener and you will gain his trust.
Example: “I see you like your coloring book! What is your favorite character in the set?”
![]()
Don’t: Change the subject during conversations.
Why: Suddenly changing the subject of conversation will negatively affect the rapport you established with your patient. He will feel that you are not paying attention to what he is saying.
Example: The patient is crying about his upcoming surgery when the nurse asks “Have you taken your pill this morning?”
Do: Acknowledge patient’s statement. When the patient becomes emotional, you can stay silent and let him express his emotions.
Example: The patient is crying about his upcoming surgery and the nurse said “I understand that this is a hard time for you. I can stay here a bit longer if that helps.”
See Also: 20 Short But Effective Prayers for Surgery
 Additional Tips – Non-Verbal Cues
Additional Tips – Non-Verbal Cues

Non-verbal cues are as important as verbal communication. Some people are more sensitive to non-verbal cues as they reflect “unspoken” thoughts.
Here are some tips on what to do and what to avoid with your gestures when interacting with your patient:
Don’ts
• Smile inappropriately – Smiling inappropriately especially in serious situations will make your patient think that you are not believing him. It also reflects a lack of attention to the ongoing conversation.
• Cross your arms or legs – Crossing your arms or legs creates a physical boundary between you and you patient. Closed posture disrupts open and spontaneous communication.
• Raise your eyebrows – Raising your eyebrows or making face during conversation leaves a negative impression with your patient. These actions imply judgmental thinking and the patient will feel uncomfortable to continue having a conversation with you.
Do’s
• Nod your head – Nodding your head while listening to your patient reflects active listening. The patient will have a non-verbal validation that you are focusing on his statements.
• Sit or stand equally – When initiating a conversation, you and your patient should be in the same level of perspective. Sit or stand at the same level with him to avoid the impression of “talking down” to him.
• Being silent for a while – The absence of verbal remarks can be therapeutic as it gives time for reflection about the ongoing conversation. It also allows the patient to think about his statements and elaborate for more.
It takes a lot of experience to be an expert in therapeutic communication. In improving your bedside manners, just keep in mind that the patient’s well-being is the primary concern in maintaining a therapeutic conversation. With this single goal in mind, your therapeutic communication skills will come out naturally from you.